Articles Cortisone Injections
This article aims to give you a good basic understanding of cortisone injections, risks and benefits.
What are Steroids?
Steroids are chemicals that are naturally produced in our bodies, they enable normal growth and function. Steroids can be categorised into 2 main groups:
Anabolic steroids, are derived from the sex organs. They help to build muscle and aid in the development of male characteristics (i.e development facial hair, deepening of voice). We often hear about these in the media due to their performance enhancing properties.

Corticosteroids, are derived from the kidneys. They act on your bodies immune system to help dampen the inflammatory response. These types of steroids are used to help alleviate the symptoms of inflammation (i.e. pain, swelling, redness, heat). They come in the form of creams, tablets, inhalable medications and injections.
Please Note: Corticosteroids should not be confused with Non-Steroidal Anti-inflammatiories (NSAIDs). NSAIDs are also widely used for their anti-inflammatory properties but act in a different way. Over the counter brands such as Advil, Neurophen, Celebrex and Voltaren are all NSAIDs.
What is a Cortisone Injection?
Cortisone injections (aka steroid injection) are typically made up of a mixture of corticosteroid and local anesthetic.
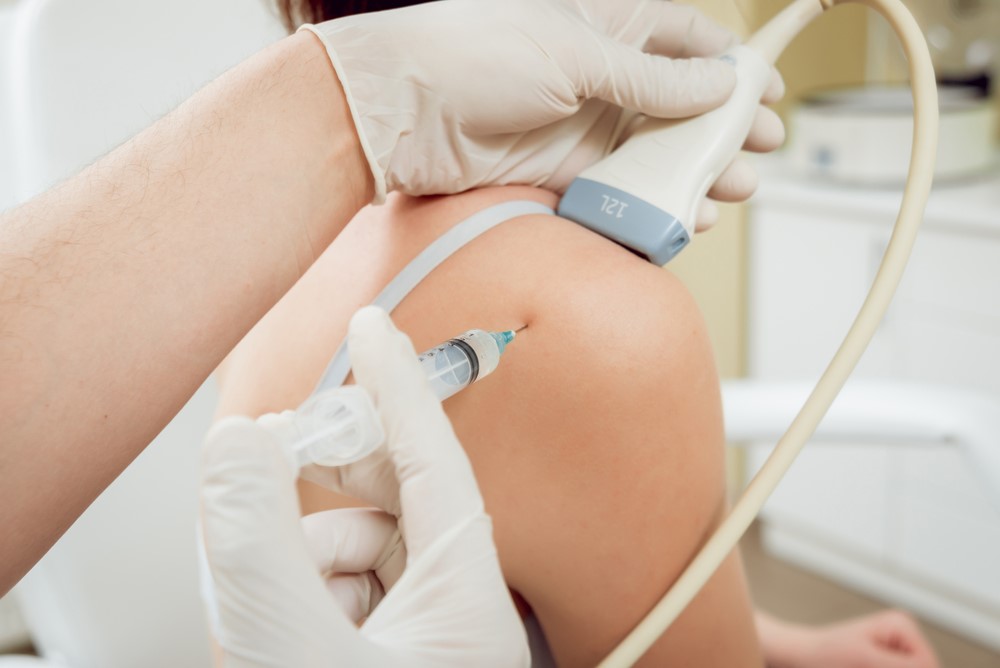
It is administered by directly injecting the solution into a localised site in the body. Image guided injections (i.e. xray, ultrasound or CT guided) are often required to ensure better accuracy. This is particularly important for more intricate structures such as the spine.
Cortisone injections are also named accordingly to where they are administered:
- facet joint injection (between the joints in the spine)
- intra-articular injection (inside a joint)
- sub-acromial injection (see image below)
- nerve root injection (spinal nerve)
- bursal injection (inside a bursa)
- intra-capsular injection (inside a joint capsule)
- epidural injection (inside a cavity in the spine)
- tendon sheath injection (inside the sheath surrounding a tendon)
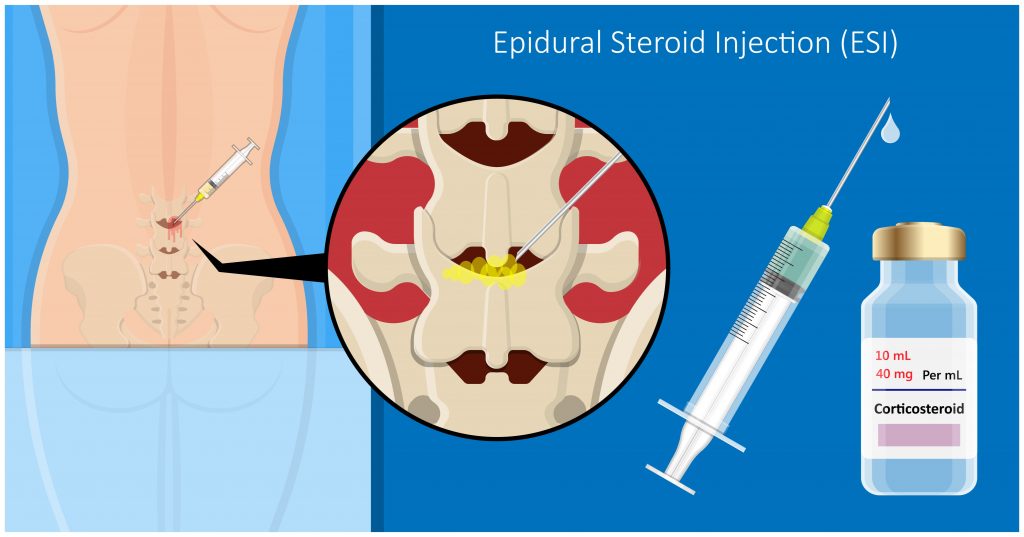
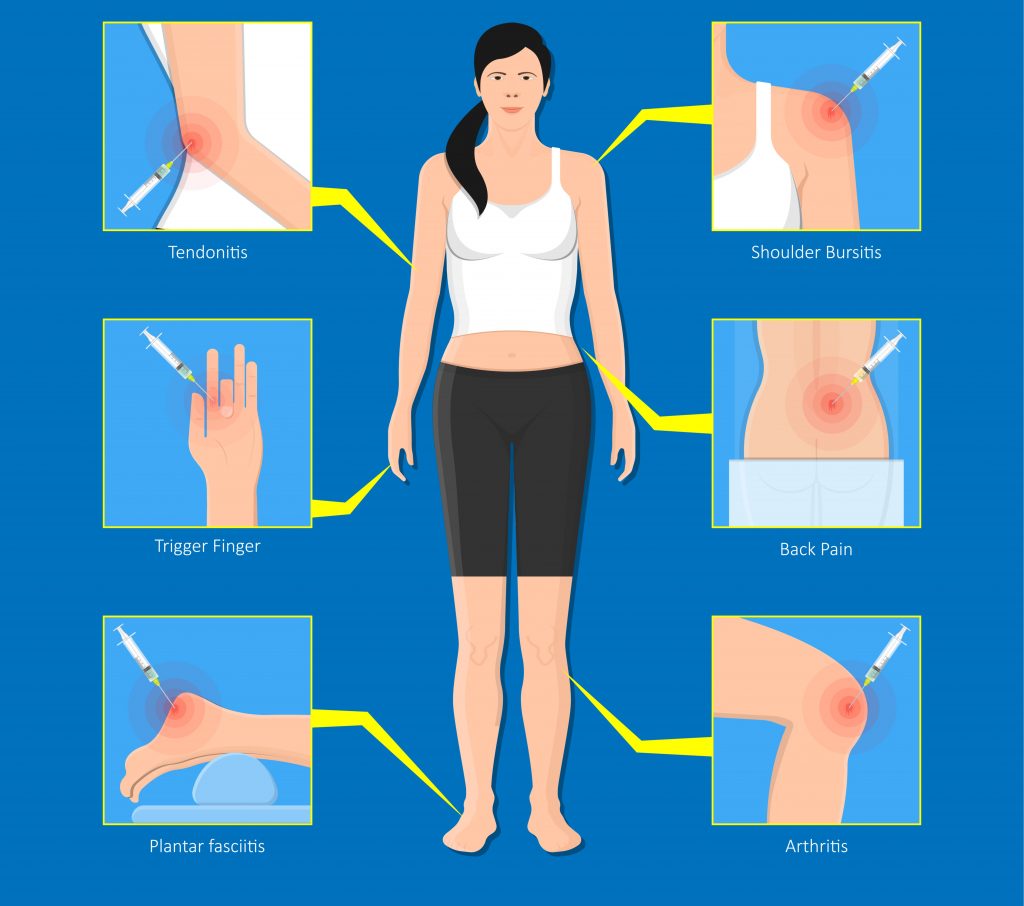
Common conditions requiring cortisone injections include :
- tendonitis
- bursitis
- nerve inflammation
- arthritic conditions (i.e. gout, rheumatoid arthritis)
- joint inflammation
- neck and back pain
Do Cortisone Injections Work?
Studies have found cortisone injections can be effective for short term pain relief (2-3 months). The long term benefits however, are questionable and it is common for injuries to reoccur which may require more than one injection. Very occasionally some people can be completely cured following a single injection, unfortunately this only constitutes a small percentage.
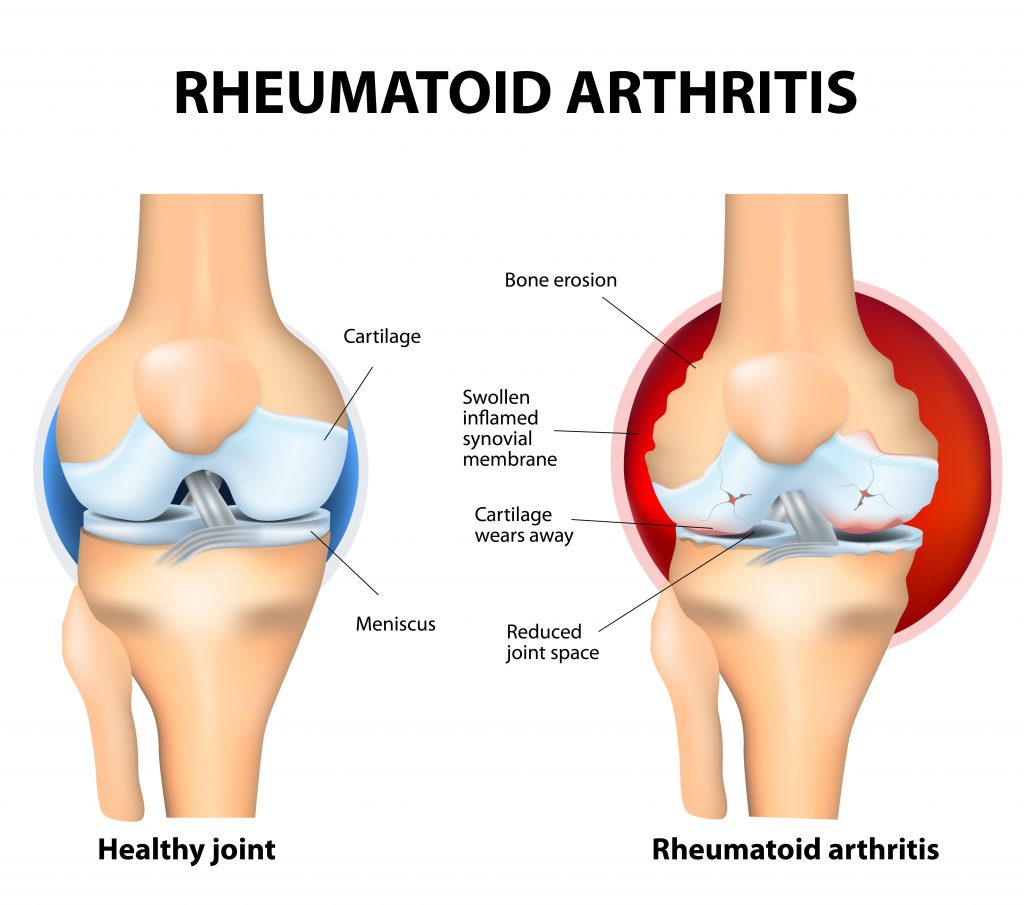
It is important to understand cortisone injections DO NOT treat the underlying cause of the injury but rather the symptoms. For Instance, inflammation of an arthritic joint is caused by break down of the joint cartilage, a cortisone injection can reduce the inflammation but will not improve the state of cartilage.
Benefits
- Quick to administer
- Potential to have quick relief of symptoms
- Relatively low risk
- Minimise the use of NSAIDs and their potential side effects (i.e. gastrointestinal upset, liver and kidney problems).
- Smaller doses of corticosteroid are required when injected into a specific site as opposed to taking tablets. This reduces potential side effects.
- Diagnostic benefits, even if the effects of a cortisone injection are short lived, it can help the practitioner to specifically identify where the problem is coming from. An accurate diagnosis enables better treatment.

Risks
- Post procedural pain, it is very common the have an exacerbation of your symptoms for 2-3 days after the procedure.
- Infection, as with any procedure that breaks the skin there is always a small risk of infection.
- Allergic reactions, the is very rare but it is very important to notify the treating practitioner of any known allergies prior to the procedure.
- Post procedural bleeding, if you have a known bleeding disorder please notify the treating practitioner.
- Raise blood sugar levels, if you are a diabetic it is important to notify the treating practitioner and monitor your blood sugar levels closely following the procedure.
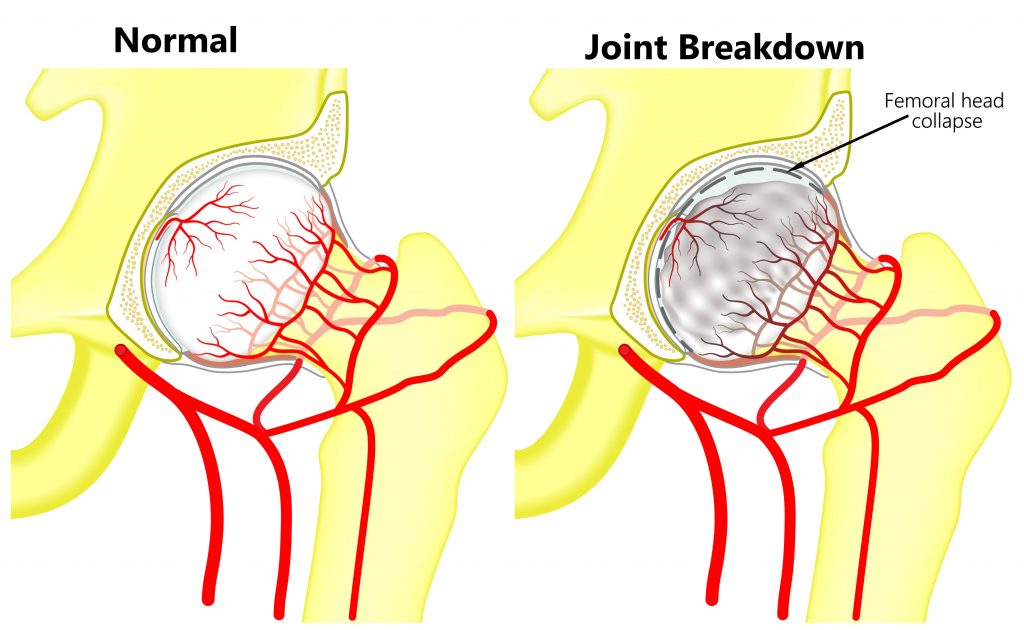
- Tissue damage, repeated cortisone injections can lead to weakening and break down of your body’s tissues (i.e skin, fat, tendons, ligaments, cartilage and bone) . To avoid this complication, it is generally recommended not to have more than 3-4 injections into the same site per year.
How Long Does it Take to Work?
Immediately following a cortisone injection many people can be completely pain free. Unfortunately, this is largely due to the local aesthetic, its effects normally wear off within 2 hours. You should know within a week whether the injection was successful or not. It is best not to overdo your exercises and activities for a few days following the injection as this can potentially aggravate the injured site.

Who Do I See to Get a Cortisone?
In Australia, cortisone injections can only be prescribed and administered by doctors (i.e. GPs, sports physicians, orthopaedic surgeons, rheumatologists and radiologists). These are not appropriate for all conditions (i.e. degenerative tendon tears, Achilles tendinitis). Your treating health professional should be able to help you weigh up the risks and benefits to decide whether a cortisone injection is the right treatment for your specific condition.
Physiotherapy Treatment
Conservative physiotherapy treatment is typically recommended prior to having a cortisone injection. This can include:
- Reducing inflammation and decreasing pain. Modalities such as RICE (Rest, Ice, Compression, Elevation), strapping, manual therapy and acupuncture may be used.
- Providing education, addressing unhelpful beliefs regarding the injury, identifying and modify aggravating factors
- Restoring pain free range of motion and preventing secondary complications
- Strengthening specific muscles and tendons to prevent recurrence of the injury.
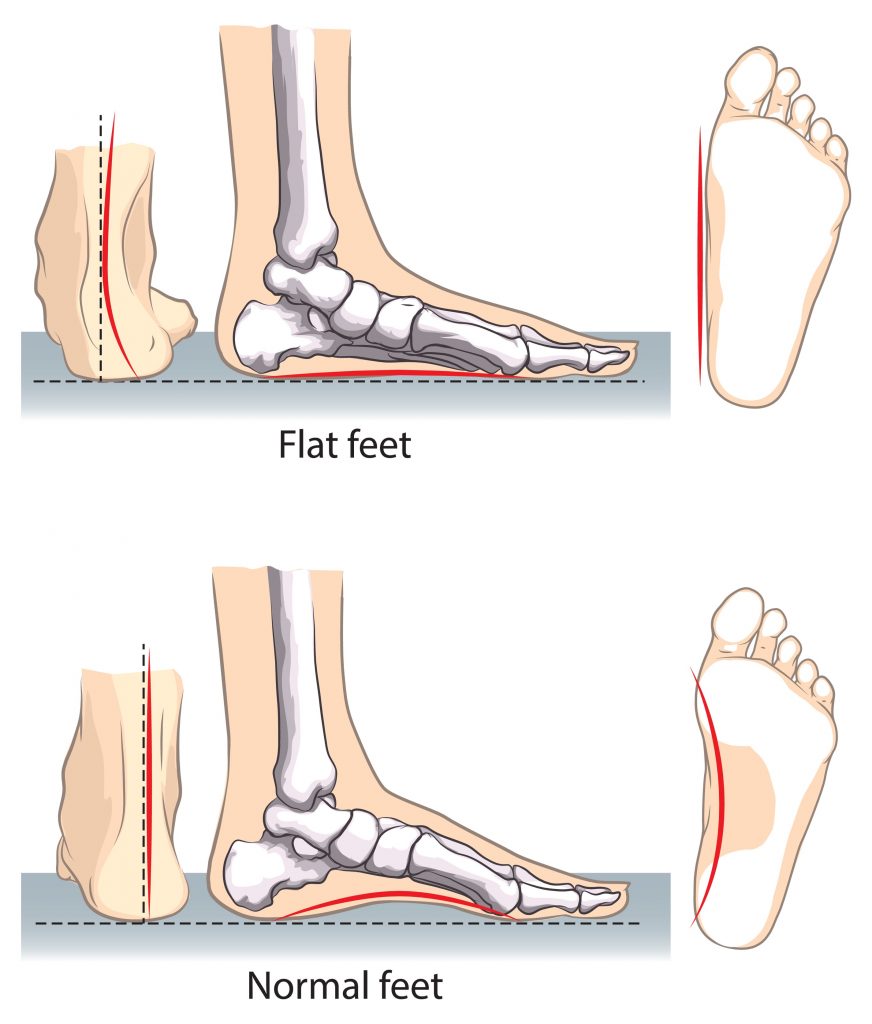
- Identifying and addressing movement and postural issues that may have contributed to the injury (i.e. flat feet, poor posture, muscle imbalances).
- Graded return to work, sport and function.
If your condition is fails to improve then a cortisone injection may be indicated. Studies have demonstrated better long term outcomes from having a cortisone injection combined with physiotherapy treatment compared to just having a cortisone injection alone
Please keep in mind the information provided is general in nature and should not be used as a substitute to consult your treating health professional. If you have any specific questions or require assistance with your individual treatment requirements please do not hesitate to contact My Family Physio Mona Vale, Northern Beaches Sydney.
Related Articles