Articles Greater Trochanteric Pain Syndrome (GTPS)
This article explains basic anatomy, what GTPS is, symptoms, causes, risk factors, diagnosis, management and physiotherapy management.
Basic Anatomy
Your thigh bone connects with your pelvis to form the hip joint.
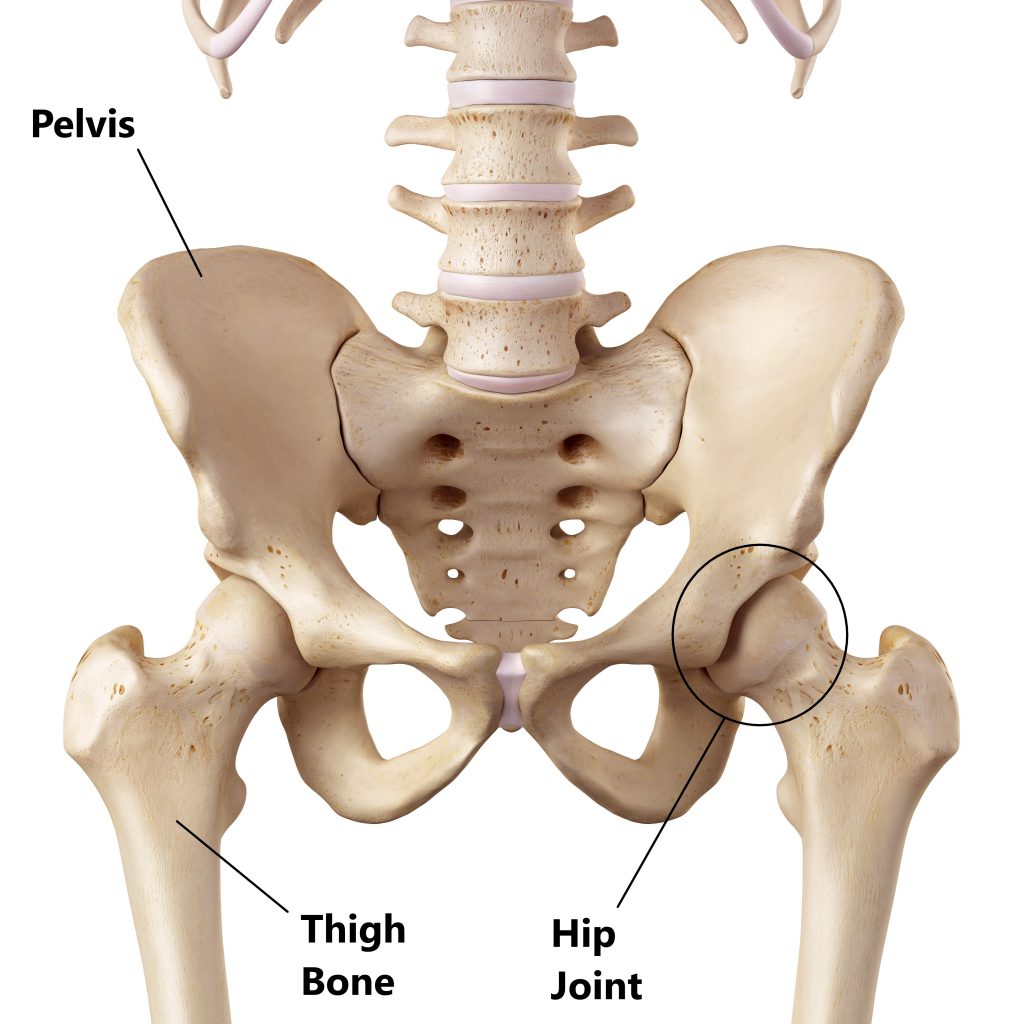
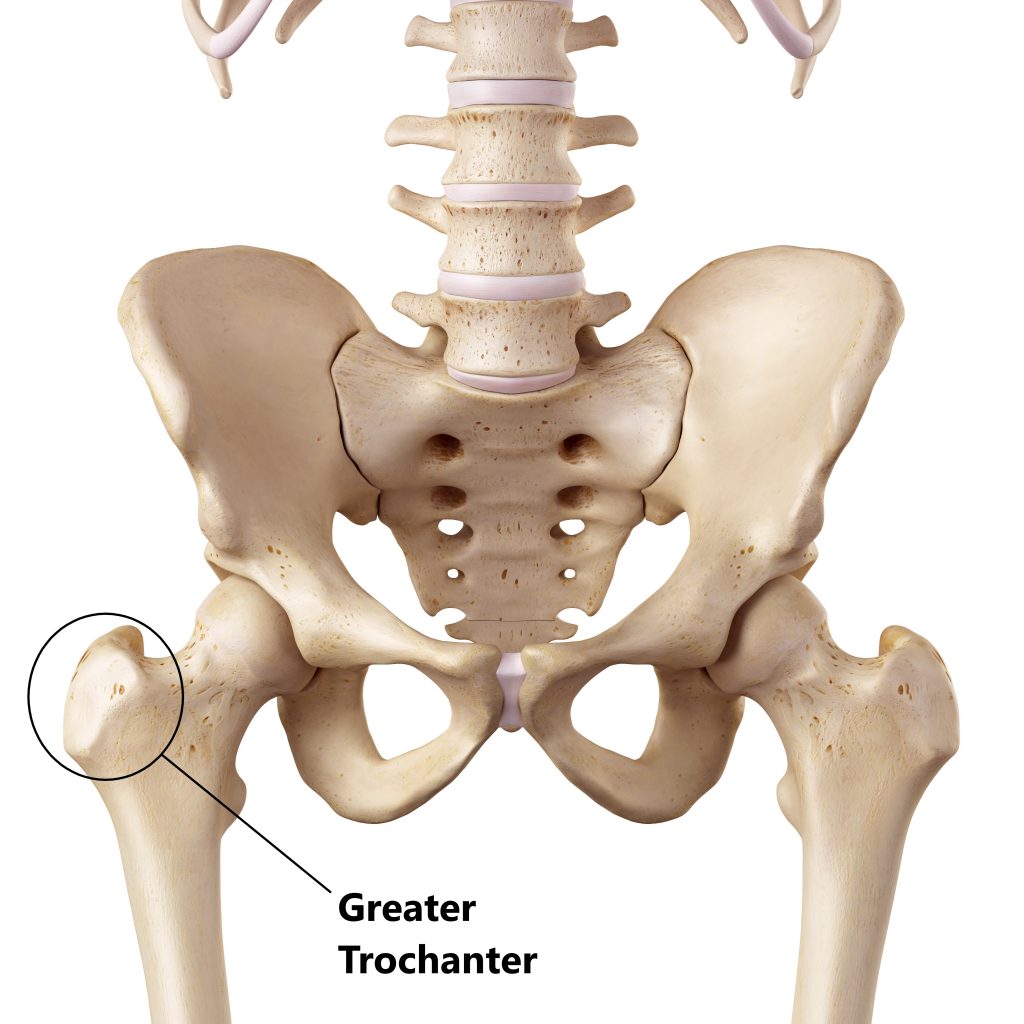
A large bony lump called the “greater trochanter” is located near the top of your thigh bone. It can be easily palpated by running your fingers up the side of your thigh over your hip.
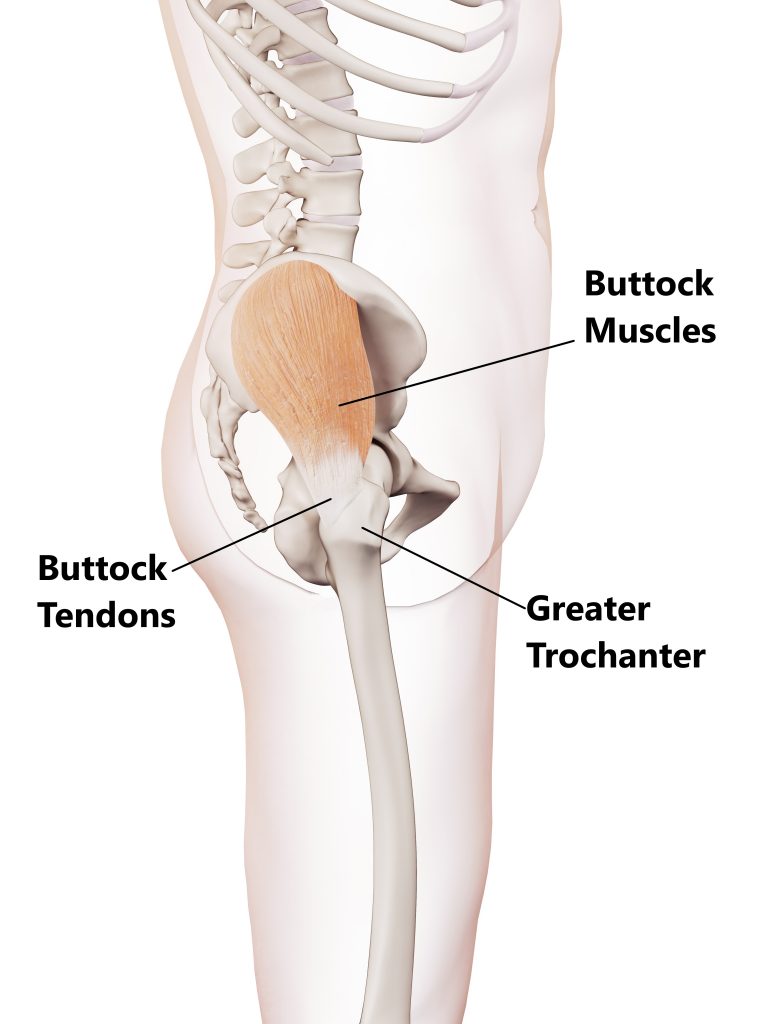
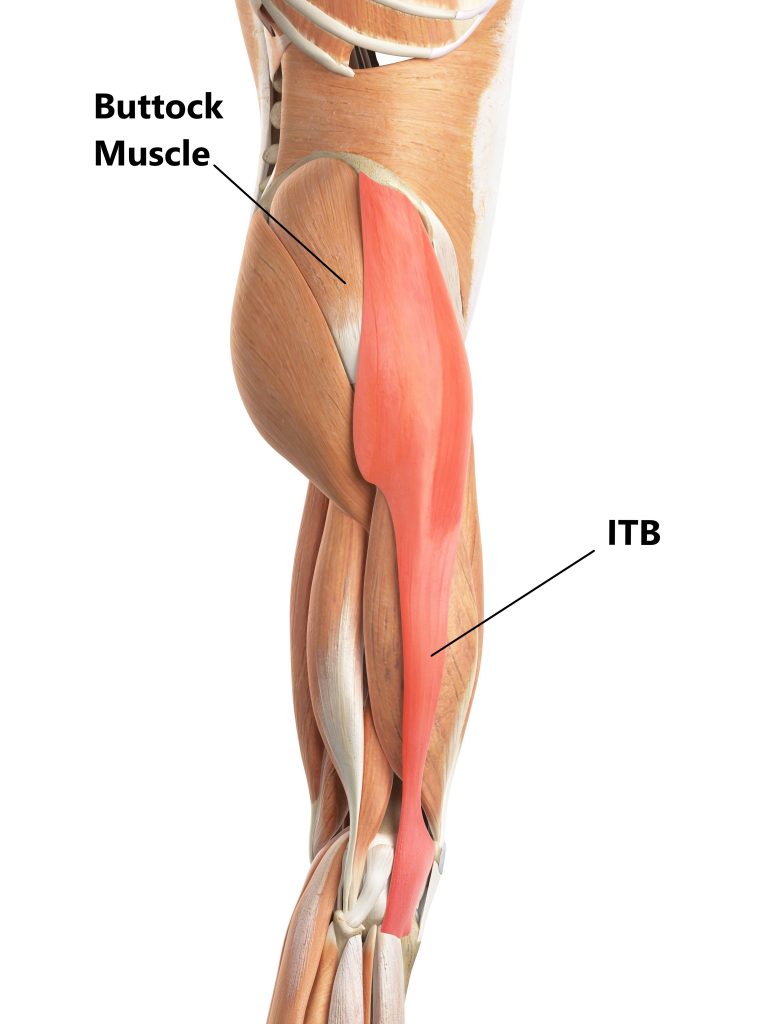
The greater trochanter is where the tendons of your buttock muscles attach to.
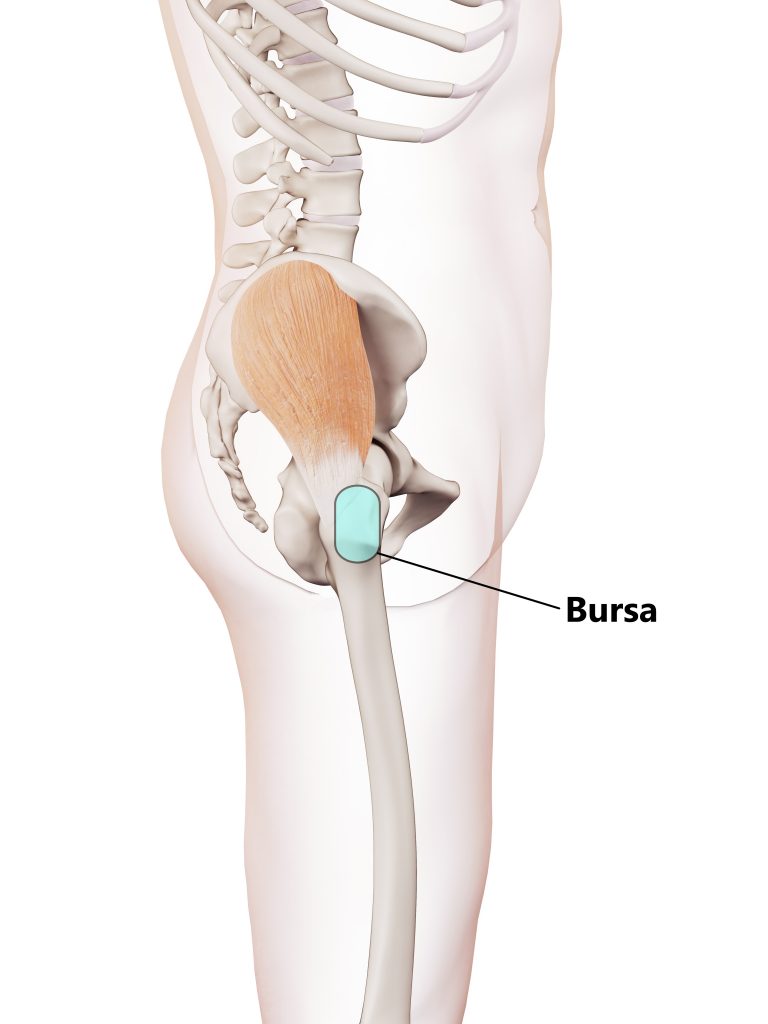
Small fluid filled sacs called bursa are located between the buttock tendons and greater trochanter to reduce friction.
Overlying all of these structures is a large inflexible sheath of tissue called the iliotibial band (ITB).
What is Greater Trochanteric Pain Syndrome (GTPS)?
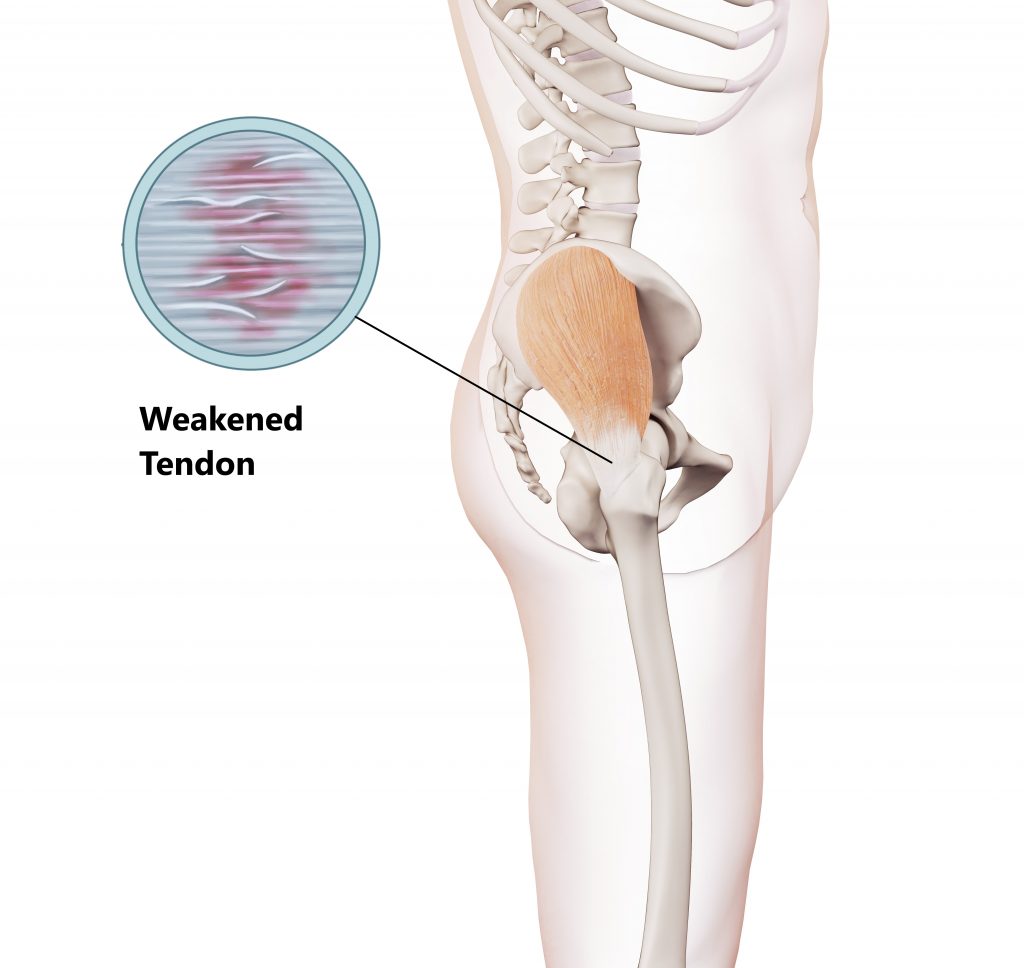
GTPS is a condition which gives rise to pain over the side of the hip. It normally involves weakening of the buttock tendons (gluteal tendinopathy) from natural wear and tear or overuse.
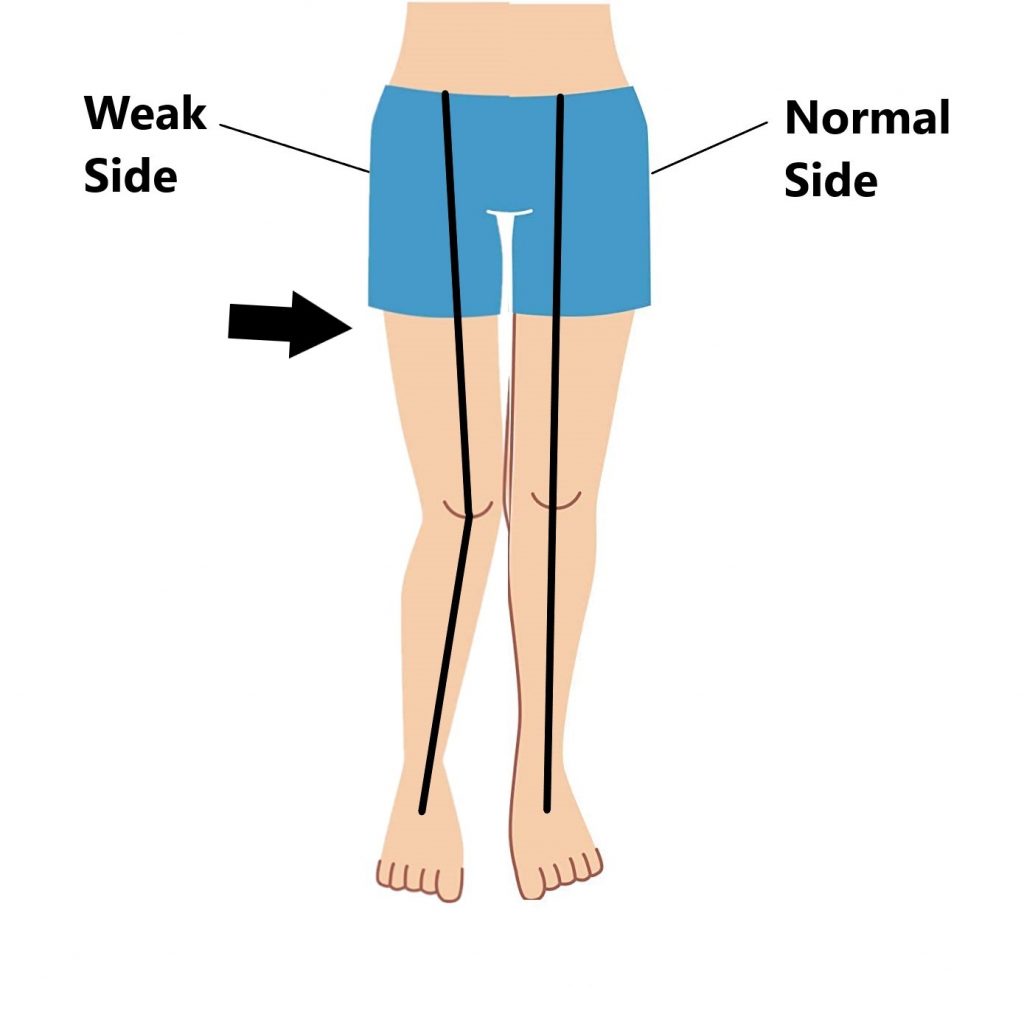
This can lead to altered positioning of the affected hip by causing it to fall inwards.
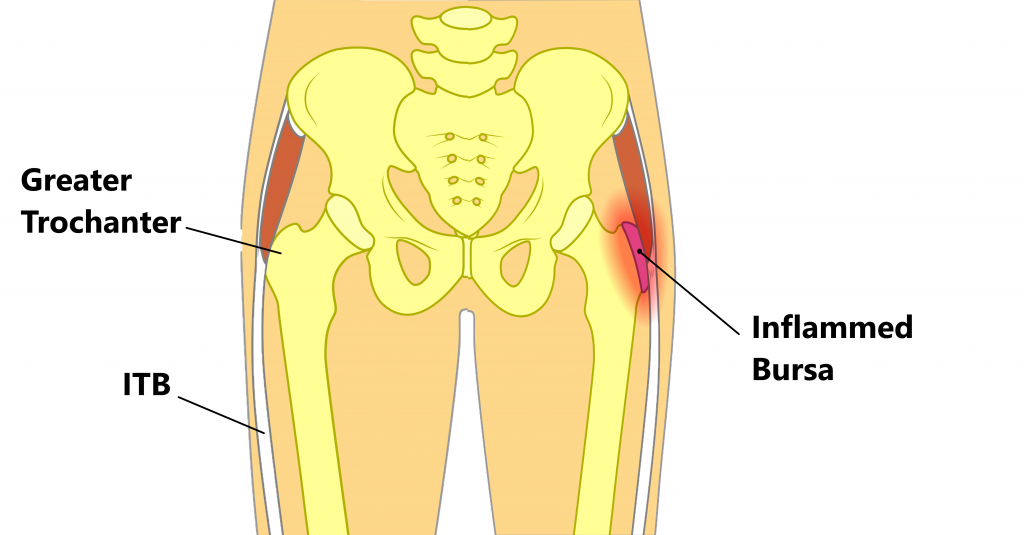
This altered position places more tension on the ITB resulting in compression and inflammation of the underlying bursa and buttock tendons.
Symptoms
- pain felt over the greater trochanter and/or side of the thigh
- tenderness on palpation over the greater trochanter
- pain when lying on the affected side, especially at night
- aggravation of symptoms with weight-bearing activities such as walking, climbing stairs, standing and running
- pain with prolonged sitting
- pain with negotiating down hill terrain and descending stairs
- pain with movements where the affected leg crosses the midline (i.e. sitting with crossed legs)
- pain with prolonged standing
Causes
- weak hip muscles /poor muscle control
- over training (i.e. ramping up running distance over a short period of time)
- commencing unaccustomed weight bearing activity (i.e. hill walking)
- falling heavily onto the side of your hip
- prolonged sitting, especially in cross legged positions or in soft deep chairs
- prolonged standing positions, especially if you tend to bear more weight on one leg
- excessive hill running
- prolonged positions requiring you to standing on one leg
- excessive abduction exercises (i.e. clams, crab walks with bands)

Risk Factors
- female gender (due to wider hips)
- individuals who are <40 years of age
- individuals who engaged in distance running
- individuals who are overweight
- individuals who have a history of lower back problems
- individuals who have a history of knee and/or hip osteoarthritis
- individuals who have uneven leg length

Diagnosis
Diagnosing this condition is mainly based on an individual’s clinical presentation through a thorough subjective and physical examination. An X-Ray or MRI may also be required to confirm the diagnosis and to exclude/identify other injuries (i.e. hip osteoarthritis).

Management
Individuals with GTPS are commonly diagnosed with hip bursitis and treated with anti inflammatory medications or a cortisone injection. Unfortunately, this approach alone often provides only short term symptomatic relief as the underlying cause of the problem (i.e. weak hip tendons) has not been addressed. Management of GTPS should be directed at both the cause and symptoms, this may include:
- physiotherapy treatment (see below)
- anti Inflammatory medications
- cortisone injection
- surgical intervention is rare and should only be considered in severe long standing cases where conservative treatment has failed
Physiotheapy Treatment
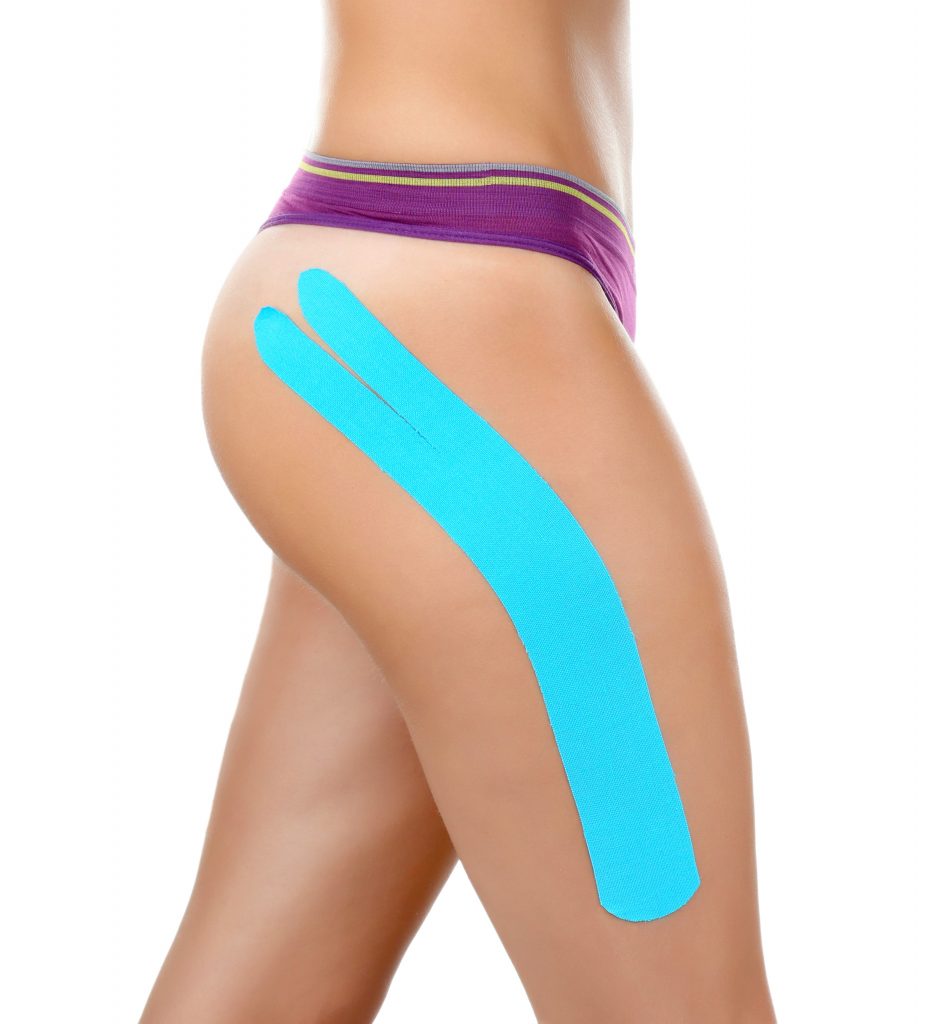
- Reduce inflammation and decrease pain. Modalities such as strapping and manual therapy may be used.
- Correction of sitting habits/postures

- Provide education regarding the injury and identify and modify aggravating factors

- Graded strengthening, particularly of the hip muscles

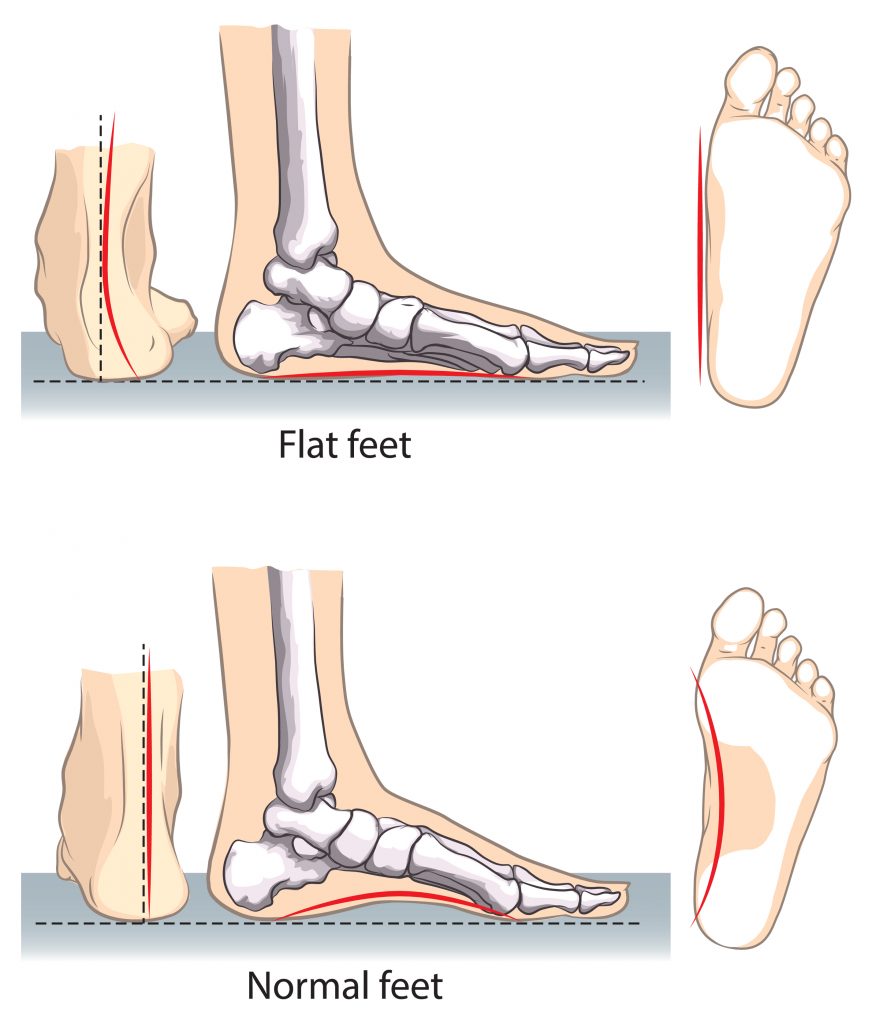
- Identify and address movement and postural issues that may have contributed to the injury (i.e. excessively flat feet, weak hip muscles, poor standing posture)
Please keep in mind the information provided is general in nature and should not be used as a substitute to consult your treating health professional. If you have any specific questions or require assistance with your individual treatment requirements please do not hesitate to contact My Family Physio, Mona Vale, NSW.